|
Case Report
Bilateral tubal pregnancy: An unusual presentation of a rare case
1 MBBS, MRCOG, Specialty Doctor, Obstetrics and Gynaecology, Mid Yorkshire NHS Teaching Trust, Wakefield, UK
2 MBBS, MRCOG, Consultant, Obstetrics and Gynaecology, Mid Yorkshire NHS Teaching Trust, Wakefield, UK
Address correspondence to:
Wynn Thi Da
Mid Yorkshire NHS Teaching Trust, Wakefield,
UK
Message to Corresponding Author
Article ID: 100163Z08YD2023
Access full text article on other devices

Access PDF of article on other devices

How to cite this article
Da WT, Wright H. Bilateral tubal pregnancy: An unusual presentation of a rare case. J Case Rep Images Obstet Gynecol 2023;9(2):43–46.ABSTRACT
Introduction: Bilateral tubal pregnancy (BTP) is the rarest form of ectopic pregnancy. The reported incidence of spontaneous BTP is 5 in 1 million deliveries.
Case Report: A 34-year-old woman with a previous diagnosis of right tubal pregnancy who had undergone surgery three weeks before presented with persistent pregnancy symptoms and abdominal pain prompting further investigation. Subsequently, bilateral tubal pregnancy was diagnosed after she underwent a second surgery for another ectopic pregnancy on the left side of the tube. Notably, both ectopic pregnancies were confirmed by histological examination.
Conclusion: This case highlights the importance of clinical awareness of the possibility of bilateral tubal pregnancy even after a patient has recently undergone surgery for an ectopic pregnancy.
Keywords: Bilateral tubal pregnancy, Ectopic, Pregnancy
Introduction
Bilateral tubal pregnancy (BTP) is an extremely rare ectopic pregnancy. The reported incidence of spontaneous BTP is 1 in 7,251,580 ectopic pregnancies and 1 in 200,000 pregnancies [1]. The actual incidence may be higher than current reports as there may be unreported cases. The first case of simultaneous BTP was reported by Collins et al. in 1912 [2].
Bilateral tubal pregnancy continues to be a clinician’s dilemma because pre-operative diagnosis is difficult and is usually made during surgery because the diagnosis is obtained retrospectively when a patient requires repeat surgery for another tubal pregnancy.
In this case, BTP was diagnosed retrospectively after the patient underwent subsequent surgery for another tubal pregnancy.
Case Report
A 34-year-old woman (G3P1+1) presented to the Emergency Department (ED) with a 1-day history of sudden sharp abdominal pain associated with vomiting and vaginal spotting. The patient developed abdominal pain in the afternoon, which worsened despite pain relief with paracetamol and codeine phosphate but denied having urinary or bowel symptoms.
The patient underwent laparoscopic right salpingectomy for a right tubal ectopic pregnancy at 5+5 weeks of gestation, three weeks before admission. The surgery was straightforward, and the patient was discharged the following day. Following surgery, the patient had persistent vomiting and abdominal distension but denied any history of sexual intercourse since surgery.
The patient had a normal vaginal delivery with her partner nine years ago and denied any pelvic inflammatory disease history. Furthermore, she was not a smoker and currently lives with a new partner.
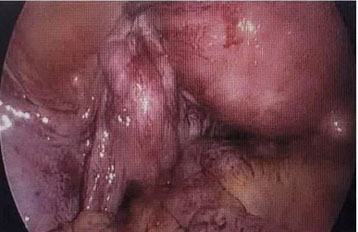
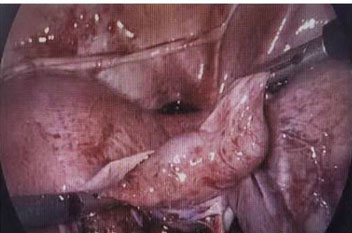
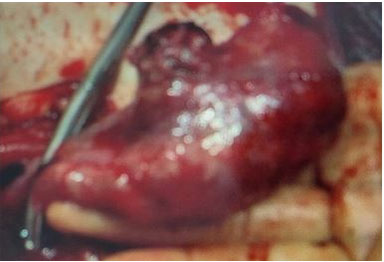
The patient had a significant history of index pregnancy and laparoscopic salpingotomy of the right fallopian tube for ectopic tubal pregnancy after the failure of medical management using one dose of methotrexate injection 18 months earlier. The operative finding at that time of surgery revealed that the left tube and ovary were adherent to the pelvic wall with filmy adhesion, and the left tube was torturous (Figure 1). As the right ectopic pregnancy was at the fimbrial end of the tube (Figure 2), a salpingotomy was performed to salvage the right tube. Beta-human chorionic gonadotropin (hCG) levels were monitored postoperatively and returned to normal.
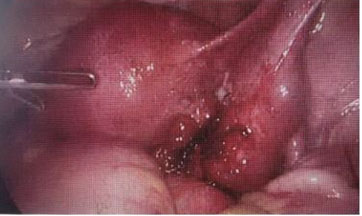
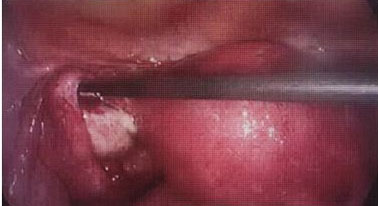
Subsequently, the patient had laparoscopic right salpingectomy at 5+5 weeks of gestation, three weeks before admission, for the recurrence of ectopic pregnancy on the same tube on the right side. The transvaginal scan revealed a pregnancy of unknown location; however, laparoscopy was performed after the working diagnosis was made based on her presenting symptoms and suboptimal fall of beta-hCG level from 3663 to 3021 IU/L at 48 hours, as well as a high index of suspicion for recurrence of ectopic pregnancy on the damaged right tube. The intraoperative findings exposed a large, unruptured right tubal ectopic pregnancy (Figure 3), a healthy left tube (Figure 4), normal ovaries, and no adhesions. Histological examination confirmed right tubal ectopic pregnancy from the presence of chorionic villi.
On examination in the ED, the patient appeared to be very dehydrated with stable vital signs: blood pressure (BP) 106/82 of mmHg and a pulse rate (PR) of 80/min. Abdominal examination revealed generalized tenderness across the suprapubic area; however, there were no signs of an acute abdomen. Speculum and vaginal examinations were unremarkable. The urine pregnancy test result was strongly positive, and leukocytes and ketones were observed. Therefore, a provisional diagnosis of vomiting with urinary tract infection was made, and the patient was admitted and treated using intravenous fluids, antiemetics, and antibiotics, with a plan for a transvaginal scan (TVS) at the department.
The patient’s hemoglobin level was 111 g/L, whereas the serum beta-hCG level was 85,000 IU/L. Transvaginal scan at the Early Pregnancy Assessment Unit the next day revealed an empty uterus and a live 8+5 week left tubal ectopic pregnancy with evidence of intra-abdominal bleeding.
The provisional diagnosis was another ectopic pregnancy in the left tube with the possibility of BTP, as the patient had a right tubal ectopic three weeks ago. However, the differential diagnosis was an abdominal pregnancy.
The repeated hemoglobin level significantly decreased from 111 at admission to 75 g/L, warranting surgical intervention. The patient was informed of another possible diagnosis of ectopic pregnancy and consented to laparoscopy, removal of the ectopic pregnancy, and peritoneal washing. Just before the surgery commenced, the hemoglobin level dropped further to 56 g/L on the HemoCue. Following the discussion with the anesthetist, the decision for laparotomy was made. The operative finding was a large ampullary ectopic pregnancy measuring approximately 10 × 8 cm (Figure 5) with 1500 mL of hemoperitoneum. Hence, a left salpingectomy was performed. The patient was debriefed postoperatively for the retrospective diagnosis of bilateral tubal ectopic pregnancy based on the sequence of events following two surgeries within three weeks: the first operation for laparoscopic right salpingectomy and the second for laparotomy and left salpingectomy. The patient received four units of blood transfusions, and the postoperative hemoglobin level was 98 g/L. The beta-hCG level repeated on the first operative day dropped to 13223 IU/L.
Discussion
A review of the available literature reveals three explanations for bilateral ectopic pregnancy: simultaneous multiple ovulations, sequential impregnation, and transperitoneal migration of trophoblastic cells from one extrauterine pregnancy to the other tube with implantation [3].
The risk factors for spontaneous BTP are similar to those for unilateral ectopic pregnancy. Moreover, it is ten-fold in women with a previous ectopic pregnancy, three-fold for those with documented tubal pathology (salpingitis secondary to sexually transmitted infections), two-fold for diethylstilbesterol (DES) exposure in utero, infertile women, those conceiving through Artificial Reproductive Technologies (ART), and smokers. However, there is a mildly increased risk for those with a history of early-age intercourse. Sterilization failure and pregnancy occurring with an intrauterine device (IUD) in situ are associated with ectopic pregnancies [4].
Fishback first suggested the criteria for diagnosing BTP in 1939, where a description of the fetuses, or any portion of them, and a description of the placental material were required to diagnose BTP. Later, Norris revised it in 1953 by stating that microscopic demonstration of chorionic villi in each tube on histopathological examination was sufficient for diagnosis [5]. In 2007, De Los Rios et al. clinically defined primary bilateral ectopic pregnancy as a condition in which at least two concurrent spontaneous pregnancies were present in the same patient, each located on the structures of the contralateral side, in the absence of an intrauterine pregnancy [6].
The clinical diagnosis of BTP is challenging because its clinical presentation is similar to that of unilateral ectopic pregnancy. Due to the wide range of serum-HCG levels during normal gestation, it is difficult to diagnose based on the serum-HCG concentration. Preoperative diagnosis by transvaginal ultrasound accurately identified bilaterality in 19% of the cases. Sonographic visualization of a unilateral ectopic pregnancy leads to complacency in assessing the contralateral tube, resulting in misdiagnosis [7]. Therefore, preoperative diagnosis is difficult, and the diagnosis is frequently made during surgery. Sometimes, the diagnosis is made only when a patient needs repeat surgery for another tubal pregnancy. Due to its rarity, the management of BTP is not discussed in the current National Institute for Health and Care Excellence (NICE) guidelines for managing ectopic pregnancy; however, the same management principles may be applied [8].
Here, the patient had a very high risk of ectopic pregnancy based on the significant history of right salpingostomy 18 months before presentation. This led to the recurrence of ectopic pregnancy at 5+5 weeks of gestation in the same right tube, where it occurred at three weeks when she underwent laparoscopic right salpingectomy before readmission to the ED.
Her unusual presentation of persistent vomiting with a non-acute abdomen on examination following surgery did not indicate another ectopic pregnancy.
Furthermore, diagnosing another ectopic pregnancy was initially a dilemma for clinicians based on the operative finding of a healthy left tube at the time of laparoscopic right salpingectomy (at 5+5 weeks of gestation) three weeks prior. On the other hand, the timeline was relevant, as the ectopic pregnancy was reported to be at 8+5 weeks of gestation. This supported the possibility of an unrecognized bilateral ectopic pregnancy on the left tube during the right salpingectomy three weeks ago. Considering that the patient was hemodynamically stable, conservative management was initially administered. However, urgent surgical intervention was performed when clinical observation deteriorated.
Conclusion
This is a very rare case of ectopic pregnancy with an unusual presentation which should not be missed if there is clinical vigilance. Careful examination of the contralateral tube during laparoscopic surgery for ectopic pregnancy is important. Clinical awareness of the rare condition of BTP is of prime importance when a patient presents with persistent symptoms of ectopic pregnancy, even after undergoing recent surgery for ectopic pregnancy. This case highlights the importance of clinical awareness of the possibility of BTP even after a patient has recently undergone surgery for an ectopic pregnancy.
REFERENCES
1.
Andrews J, Farrell S, Andrews J. Spontaneous bilateral tubal pregnancies: A case report. J Obstet Gynaecol Can 2008;30(1):51–4. [CrossRef]
[Pubmed]

2.
Collins ET. Double ruptured ectopic gestations. Proc R Soc Med 1912;5(Obstet Gynaecol Sect):374.
[Pubmed]

3.
Tabachnikoff RM, Dada MO, Woods RJ, Rohere D, Myers CP. Bilateral tubal pregnancy. A report of an unusual case. J Reprod Med 1998;43(8):707–9.
[Pubmed]

4.
5.
Norris S. Bilateral simultaneous tubal pregnancy. Can Med Assoc J 1953;68(4):379–81.
[Pubmed]

6.
De Los Ríos JF, Castañeda JD, Miryam A. Bilateral ectopic pregnancy. J Minim Invasive Gynecol 2007;14(4):419–27.
[Pubmed]

7.
Arcilla MRC, Sapaula MS, Barrientos MA, Fernandez MA. Primary bilateral tubal pregnancy: A case report and review of literature. [Available at: https://api.semanticscholar.org/CorpusID:248825766]

8.
National Institute for Health and Care Excellence. Ectopic pregnancy and miscarriage: Diagnosis and initial management. London: NICE; 2019. (Clinical guideline [NG126]). [Available at: https://www.nice.org.uk/guidance/ng126]