|
Case Report
Vesicouterine fistula following multiple cesarean sections: A case report
1 Department of Obstetrics and Gynecology Kasserine, Sousse University, Kasserine Maternity Center, Tunisia
Address correspondence to:
Montacer Hafsi
Medical Resident in Gynecology and Obstetrics,
Message to Corresponding Author
Article ID: 100189Z08MH2024
Access full text article on other devices

Access PDF of article on other devices

How to cite this article
Hafsi M, Zouaghi A, Rhimi K, Ltifi B, Jellali N, Gharsalli R, Armi S. Vesicouterine fistula following multiple cesarean sections: A case report. J Case Rep Images Obstet Gynecol 2024;10(2):62–65.ABSTRACT
Introduction: Vesicouterine fistula, also known as Youssef’s syndrome, is a rare but significant complication primarily arising after cesarean sections. This condition involves an abnormal connection between the bladder and the uterus, which can lead to symptoms such as cyclic hematuria (menstrual blood in the urine) and urinary leakage. The increasing incidence of cesarean deliveries highlights the need for greater awareness and effective management of this condition.
Case Report: We present the case of a 32-year-old woman with a history of multiple cesarean sections who was admitted with spontaneous labor at 36 weeks and 4 days of amenorrhea. Initial diagnostic imaging and clinical assessment indicated a viable pregnancy but revealed a history of extensive intra-abdominal adhesions. During an emergency cesarean section, complications included a bladder injury and a 2 cm uterine rupture. Post-operatively, the persistent presence of hematuria led to further investigation using retrograde urethrocystography (UCR), which confirmed the diagnosis of a vesicouterine fistula. The diagnosis of vesicouterine fistula presents significant challenges due to its rarity and the overlap of symptoms with other conditions such as malignancies or bladder injuries. The condition is often associated with difficult cesarean sections and extensive intra-abdominal adhesions. Accurate diagnosis relies on imaging techniques, particularly UCR, to identify the fistula and guide appropriate surgical intervention. Effective management includes careful surgical repair and post-operative monitoring to resolve the fistula and restore normal bladder and uterine function.
Conclusion: Vesicouterine fistula is a rare but important complication following cesarean sections, requiring prompt recognition, and management. Awareness of its symptoms and the potential for occurrence in patients with a history of multiple cesarean deliveries is essential for early diagnosis. Imaging modalities, such as UCR, are crucial for accurate diagnosis and guiding surgical treatment. Early intervention and careful post-operative care are key to achieving favorable outcomes and preserving reproductive health.
Keywords: Bladder injury, Cesarean section, Intra-abdominal adhesions, Vesicouterine fistula, Youssef’s syndrome
Introduction
Youssef’s syndrome, characterized by a vesicouterine fistula that traverses the isthmus of the uterus, is a rare but significant complication in obstetric practice. This type of fistula accounts for approximately 4% of all urogenital fistulas and predominantly affects young women of reproductive age. The condition arises when an abnormal connection forms between the bladder and the uterus, allowing menstrual blood to flow into the bladder and resulting in symptoms such as cyclic hematuria and urinary leakage.
Typically, Youssef’s syndrome develops as a complication of a challenging cesarean section. The fistula often arises from surgical difficulties, such as excessive tissue damage, excessive bleeding, or intra-abdominal adhesions that complicate the procedure. Understanding the etiology and presentation of this syndrome is crucial for early diagnosis and effective management, which can significantly impact patient outcomes and quality of life.
Case Report
A 32-year-old woman, Rh-positive blood type A, with a history of five pregnancies and five deliveries (G5P5) and an extensively scarred uterus, was urgently transferred to our service due to the onset of spontaneous labor at 36 weeks and 4 days of amenorrhea. This pregnancy had not been monitored, making her clinical situation more complex.
Upon examination, the patient’s blood pressure was within normal limits. Uterine contractions were present and rhythmic, with the uterus relaxing between contractions. The fetal heart rate was normal, demonstrating appropriate variability and reactivity. A vaginal examination revealed a cervix dilated to 3 cm, 80% effaced, with a cephalic presentation and an intact amniotic sac. Obstetric ultrasound confirmed a viable pregnancy with positive fetal cardiac activity and a placenta positioned away from the uterine scar, indicating no immediate placental complications.
Given the patient’s condition, she was swiftly transferred to the operating room for an emergency cesarean section. During the surgical procedure, the Pfannenstiel incision from previous cesareans was reopened. The operative findings included significant uterine-to-parietal adhesions and an elevated bladder. The surgical team performed careful adhesiolysis to release the adhered tissues, gently detached the uterovesical peritoneum, and lowered the bladder to gain access to the underlying structures.
These interventions revealed a 2 cm uterine rupture at the site of the old scar, complicating the cesarean section. Despite these challenges, a successful cephalic delivery of a female newborn weighing 2650 grams was achieved. The newborn had Apgar scores of 7, 8, and 9 at 1, 5, and 10 minutes, respectively, indicating a good initial adaptation to extrauterine life.
Following delivery, the presence of hematuria (blood in the urine) was noted, prompting further investigation. A blue dye test was performed, which confirmed the presence of a bladder dome injury. The urologist repaired the bladder injury in two layers and placed a permanent 20 French urinary catheter to facilitate healing and ensure proper urinary drainage.
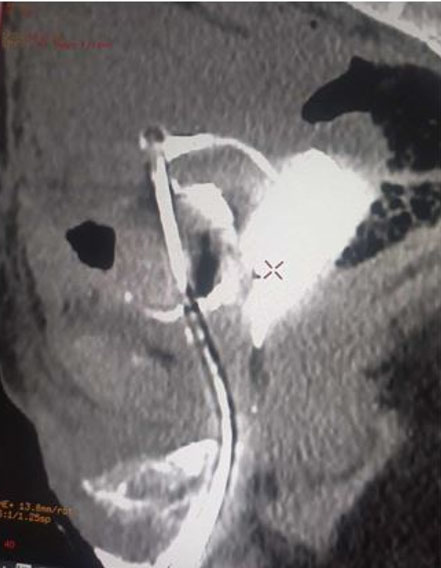
Three weeks later, a follow-up with the urologist showed persistent hematuria. To further investigate the cause, a retrograde urethrocystography (UCR) was conducted, revealing the presence of a vesicouterine fistula. This abnormal connection between the bladder and the uterus necessitated additional surgical intervention (Figure 1 and Figure 2). The patient is now scheduled for surgical revision to address and repair the vesicouterine fistula and to manage the resulting complications.
Discussion
The first documented case of a vesicouterine fistula was described by Knipe et al. in 1908 [1],[2]. However, it was not until 1957 that the Egyptian physician Abdel Fattah Youssef introduced the term “menourie” to describe this condition [3]. Youssef’s syndrome is characterized by a triad of symptoms: cyclic hematuria (or menourie), amenorrhea, and complete urinary continence [2],[3]. This syndrome is thought to be associated with the presence of a cervico-isthmic uterine sphincter, which allows the fistula to function unidirectionally from the uterus to the bladder [4].
Since 1974, fewer than 55 cases of Youssef’s syndrome have been reported in the medical literature [2]. The development of this condition is closely linked to bladder trauma, with lower segment cesarean sections being the primary identified cause [1],[2],[4]. The risk of developing Youssef’s syndrome is particularly high in cases involving difficult uterine dissection or uterine rupture. This risk is notably increased in repeated cesarean sections, such as in our reported case.
Other potential causes include extension of the hysterotomy during a difficult fetal extraction, transvesical cesarean sections, or transfixation of the bladder during hysteropexy. Additionally, other etiologies have been reported in the literature, including pelvic tuberculosis, degenerated fibroids, and actinomycosis following the prolonged insertion of an unreplaced intrauterine device [1].
From a pathophysiological perspective, one might expect the fistula to allow bidirectional flow between the bladder and the uterus, manifesting as both cyclic hematuria and urinary leakage. However, numerous cases of “unidirectional” vesicouterine fistulas with perfect urinary continence have been documented [5],[6]. The exact mechanism remains controversial, but it is believed that the tone of the uterine isthmus after delivery plays a crucial role in the clinical presentation of Youssef’s syndrome. When this tone is properly restored, menstrual blood more easily flows into the bladder, which has a lower pressure, thus explaining the absence of urinary leakage through the vagina, menourie, and amenorrhea [4],[5],[6].
Typically, Youssef’s syndrome presents with a triad of menourie, amenorrhea, and urinary continence, although this classic presentation is rare. Symptoms can vary over time within the same patient, sometimes showing successive phases of “bidirectional” symptoms: initially urinary leakage, followed by cyclic hematuria, and then complete urinary continence [6]. In our case, despite the repair of the bladder injury and placement of a large-caliber urinary catheter, the patient experienced hematuria for three weeks.
The clinical examination with methylene blue bladder filling can diagnose the fistula by observing leakage of the dye from the cervical area. However, false negatives can occur, emphasizing the need for supplementary diagnostic tests. Intravenous urography, commonly used in literature, can diagnose vesicouterine fistula (FVU) by demonstrating contrast passage into the uterine cavity and ruling out associated ureteral injuries [1]. When intravenous urography yields inconclusive results, retrograde urethrocystography (UCR) is typically performed to reveal the fistulous tract [5], as observed in our patient.
Surgical treatment for vesicouterine fistulas is most commonly performed through transvesical, retroperitoneal, or transperitoneal approaches. Ideally, this surgery is delayed for three months after the initial injury to allow for proper healing and stabilization of the lesions, minimizing risks related to edema and persistent inflammation. The intervention involves a vesicouterine separation with separate suturing of the uterus and bladder using absorbable stitches, with or without the interposition of omentum or vesicouterine peritoneum to reinforce the sutures [1],[4]. Endoscopic fulguration of the bladder fistula orifice is another described method but requires bladder drainage for two weeks and has a high failure rate [1],[4].
Conclusion
Youssef’s syndrome, a clinical manifestation of vesicouterine fistulas (FVU), is a rare but increasingly recognized obstetric complication, particularly with the rise in cesarean deliveries. This syndrome most commonly arises from cesarean sections, uterine ruptures, hysterectomies, or instrumental manipulations. The primary treatment for Youssef’s syndrome is surgical intervention.
Prevention is crucial and can significantly mitigate the risk of developing this syndrome. Key preventative measures include: placing a urinary catheter before any cesarean delivery, carefully managing vesicouterine adhesions, ensuring thorough dissection of the vesicouterine space prior to any uterine incision, conducting a bladder integrity test, and repairing any bladder injuries with appropriate post-operative bladder drainage lasting at least 10 days. By adhering to these precautions, the incidence of Youssef’s syndrome and its associated complications can be effectively reduced.
REFERENCES
1.
Mohammed B, Paul OJ, Mustapha A, et al. Urinary incontinence revealing vescicouterine fistula: About a case. [Article in French]. Pan Afr Med J 2018;31:32. [CrossRef]
[Pubmed]

2.
Kettache R, Merad A, Buchholz NNP. Surgical management of Youssef's syndrome: A case report. Urol Int 2020;104(9–10):833–6. [CrossRef]
[Pubmed]

3.
Youssef AF. Menouria following lower segment cesarean section; A syndrome. Am J Obstet Gynecol 1957;73(4):759–67. [CrossRef]
[Pubmed]

4.
el Fassi Fassi MJ, Tazi K, Karmouni T, et al. Youssef syndrome (vesico-uterine fistula): Three case reports. [Article in French]. Ann Urol (Paris) 2003;37(4):184–6. [CrossRef]
[Pubmed]

5.
SUPPORTING INFORMATION
Author Contributions
Montacer Hafsi - Conception of the work, Design of the work, Acquisition of data, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Asma Zouaghi - Conception of the work, Design of the work, Drafting the work, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Kawther Rhimi - Conception of the work, Design of the work, Drafting the work, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Besma Ltifi - Acquisition of data, Drafting the work, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Nejmeddine Jellali - Conception of the work, Design of the work, Drafting the work, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Rachid Gharsalli - Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Sawssem Armi - Conception of the work, Design of the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Guaranter of SubmissionThe corresponding author is the guarantor of submission.
Source of SupportNone
Consent StatementWritten informed consent was obtained from the patient for publication of this article.
Data AvailabilityAll relevant data are within the paper and its Supporting Information files.
Conflict of InterestAuthors declare no conflict of interest.
Copyright© 2024 Montacer Hafsi et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information.