|
Case Report
A spontaneous epidermal inclusion cyst of the vulva: A case report
1 Department of Obstetrics and Gynecology, King Abdulaziz Medical City, National Guard Health Affairs, Riyadh, Saudi Arabia
Address correspondence to:
Wafa Alshahrani
Department of Obstetrics and Gynecology, King Abdulaziz Medical City, National Guard Health Affairs, Riyadh,
Saudi Arabia
Message to Corresponding Author
Article ID: 100210Z08WA2025
Access full text article on other devices

Access PDF of article on other devices

How to cite this article
Alshahrani W, Hijazi A. A spontaneous epidermal inclusion cyst of the vulva: A case report. J Case Rep Images Obstet Gynecol 2025;11(2):5–7.ABSTRACT
Introduction: Epidermal inclusion cyst can occur in multiple parts of the body including the female genitals. Most cases occur in women with past surgical procedure done including female genital mutualization or episiotomy. We present here a case of epidermal inclusion cyst with no history of valvular surgery or trauma.
Case Report: A 24-year-old lady who presented to the clinic complaining of a slow growing mass which has affected her daily life due to its size. Upon examination, 8 × 5 cm palpable and nontender mass was noted. Surgical excision was done to the mass and tissue was sent for histopathology.
Conclusion: Epidermal inclusion cyst should always be considering a differential diagnosis in cases of valvular mass.
Keywords: Clitoral mass, Epidermal cyst, Valvular mass, Vulvar tumor
Introduction
Epidermal vulvar cysts are rarely seen. The majority of these cysts are asymptomatic and slow-growing round tumors, which can occur in any part of the body, including the face, neck, trunk, and external genitalia. When affecting the external genitalia in female, they mainly appear in the vulval or clitoral region [1],[2]. Examples for benign vulvar cysts include Bartholin’s cyst, endometrioma, lipoma, and epidermal cyst [3]. Vulvar epidermal cysts are mostly reported in women, mainly in the clitoris, and in women who have suffered trauma to the genital area, such as female genital mutilation [4]. The definitive diagnosis is determined by histopathological results obtained during surgery. Herein, we present a case of a young lady who was diagnosed with epidermal inclusion cyst and had no surgeries done to the vulva prior to her presentation.
Case Report
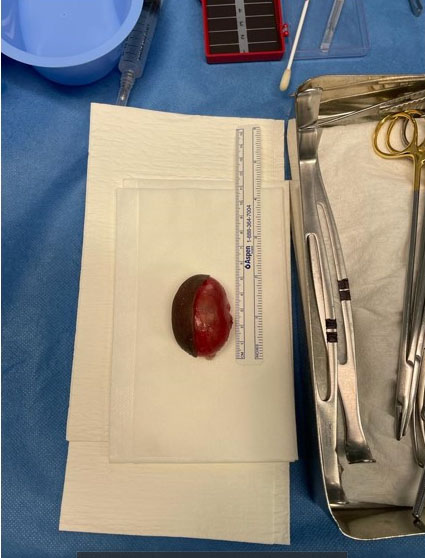
A 24-year-old, single female, who is not known to have any medical diseases, presented to the gynecology out-patient clinic complaining of swelling in the genital area which has increased in size over the past year. She was a virgin and had no history of previous genital trauma or surgery. Upon examination, a mass was noted, measuring 8 × 5 cm, the mass was arising from the clitoral area, and extended between the two labia majora. The mass was cystic, round and nontender. The patient was counseled and booked for cystectomy as an elective procedure. Intraoperatively, the mass was well demarcated, distinct from the clitoris and the urinary meatus (Figure 1). The cyst was excised completely and was found to be filled with thick yellow “cheesy” material” (Figure 2). The cyst was sent for histopathology with the report indicating an epidermal inclusion cyst. The postoperative recovery course was uneventful, and the patient was sent home on the same day.
Discussion
Epidermal inclusion cyst can occur in different parts of the body including the face, genitals, extremities, and trunk. Most of the reported cases of epidermal inclusion cyst in the female genitalia are localized to the clitoris. Epidermal cysts arise from the displacement of the epidermis into the dermis or subcutaneous tissue. In most cases, epidermal cysts occur in women with previous history of trauma or surgery to the genitals; however, few cases were reported in the literature describing women denying any past surgical history or trauma as in our case [5],[6] Patients mainly present to the clinic with a history of a slow growing painless mass which leads to difficulty in walking and sitting down [6]. The largest diameter which has been reported is 12 cm [7].
History and examination are great tools in narrowing down the differential diagnosis. Differential diagnosis of vulvar benign tumor includes Bartholin cyst, cyst of the canal of Nuck, lipoma, endometrioma, and epidermal inclusion cyst. Although rare, malignant tumors such as liposarcoma must be considered as a differential diagnosis [6],[8],[9]. In terms of imaging, magnetic resonance imaging (MRI) is superior in differentiating underlying extension of the tissue and the mass location. Compared to other types of cysts, epidermal inclusion cysts tend to be hyperintense on diffuse weight images in MRI scan. Some authors have believed that small masses can be followed up by radiological and clinical assessment. However, in large masses such our case, surgical intervention is the treatment of choice [6].
Surgical resection treatment in cases of vulvar cysts helps relieve the symptoms and the mass tissue can be sent for histopathology [10]. During surgery, surgeons must be alert to the possibility of having profound bleeding in case the mass was extending deep into the clitoris or into the inferior hemorrhoidal branch of the pudendal vessels. To reach a satisfying cosmetic outcome, proper dissection and closure of the wound with no tension are mandatory [7].
Conclusion
Epidermal Inclusion cysts can occur in different parts of the body. When occurring in the genital area, it mainly occurs in the labia majora especially at the clitoris. Definitive diagnosis can only be achieved through histopathology after surgical excision. Magnetic resonance imaging is beneficial in some cases to help in the differential diagnosis. Surgical intervention carries a good prognosis and cosmetic results.
REFERENCES
1.
Schmidt A, Lang U, Kiess W. Epidermal cyst of the clitoris: A rare cause of clitorimegaly. Eur J Obstet Gynecol Reprod Biol 1999;87(2):163–5. [CrossRef]
[Pubmed]

2.
Saha M. Epidermoid cyst of the clitoris: A rare cause of clitoromegaly. APSP J Case Rep 20134;4(3):51.
[Pubmed]

3.
Zuker N. Unusual epidermal cyst of the vulva. Aust N Z J Obstet Gynaecol 1996;36(1):111. [CrossRef]
[Pubmed]

4.
Kroll GL, Miller L. Vulvar epithelial inclusion cyst as a late complication of childhood female traditional genital surgery. Am J Obstet Gynecol 2000;183(2):509–10. [CrossRef]
[Pubmed]

5.
Gupta S, Gupta S, Jain VK, Kumar B. A “stone” in the vulva. Sex Transm Infect 2000;76(4):319. [CrossRef]
[Pubmed]

6.
Yang WC, Huang WC, Yang JM, Lee FK. Successful management of a giant primary epidermoid cyst arising in the labia majora. Taiwan J Obstet Gynecol 2012;51(1):112–4. [CrossRef]
[Pubmed]

7.
8.
Isaacson D, Turner ML. Localized vulvar syringomas. J Am Acad Dermatol 1979;1(4):352–6. [CrossRef]
[Pubmed]

9.
Larrabee R, Kylander DJ. Benign vulvar disorders. Identifying features, practical management of nonneoplastic conditions and tumors. Postgrad Med 2001;109(5):151–4, 157–9, 163–4. [CrossRef]
[Pubmed]

10.
Nucci MR, Fletcher CD. Liposarcoma (atypical lipomatous tumors) of the vulva: A clinicopathologic study of six cases. Int J Gynecol Pathol 1998;17(1):17–23. [CrossRef]
[Pubmed]

SUPPORTING INFORMATION
Author Contributions
Wafa Alshahrani - Conception of the work, Design of the work, Acquisition of data, Drafting the work, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Ayah Hijazi - Conception of the work, Design of the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Guaranter of SubmissionThe corresponding author is the guarantor of submission.
Source of SupportNone
Consent StatementWritten informed consent was obtained from the patient for publication of this article.
Data AvailabilityAll relevant data are within the paper and its Supporting Information files.
Conflict of InterestAuthors declare no conflict of interest.
Copyright© 2025 Wafa Alshahrani et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information.