|
Clinical Image
Cyclically bleeding umbilical mass: A case of primary umbilical endometriosis
1 School of Medicine, University of Hawaii John A. Burns School of Medicine, Honolulu, HI, USA
2 Department of Surgery, Oregon Health and Sciences University, Portland, OR, USA
3 Department of Family Medicine and Community Health, University of Hawaii John A. Burns School of Medicine, Honolulu, HI, USA
Address correspondence to:
Komal Soin
MD, MPH, Department of Family Medicine and Community Health, University of Hawaii, Pali Momi Outpatient Center, 98-1005 Moanalua Rd Spc 3030, Aiea, HI 96701,
USA
Message to Corresponding Author
Article ID: 100220Z08JH2025
Access full text article on other devices

Access PDF of article on other devices

How to cite this article
Huang J, Lu M, Soin K. Cyclically bleeding umbilical mass: A case of primary umbilical endometriosis. J Case Rep Images Obstet Gynecol 2025;11(2):55–58.ABSTRACT
No Abstract
Keywords: Cutaneous endometriosis, Cyclical bleeding, Dysmenorrhea, Umbilical endometriosis, Umbilical mass
Case Report
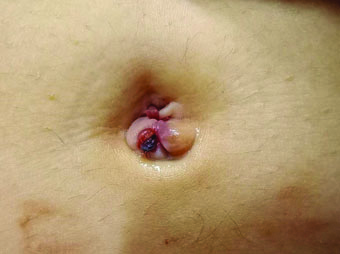
A 28-year-old woman presented initially to an urgent care clinic with a small mass protruding out of the umbilicus. The lesion was diagnosed as a skin tag and excised with minimal bleeding. Eight months later, she presented to our family medicine clinic for the growth of two similar masses in the umbilicus that now exuded blood. They were characterized as fibrous skin-colored papules and were associated with mild pain and pruritus (Figure 1).
Upon examination, there was no tenderness to palpation, no deep abdominal pain, no nausea or vomiting, no purulent discharge from the site, and no fever, flank pain, or dysuria. The patient denied any history of trauma to the area. The patient has no significant past medical history. She has a negative family history of melanoma and other skin cancers. At this time, the patient was referred to dermatology for a recurring skin lesion.
After the visit, via secure digital communication, the patient later noted that the onset of bleeding from the umbilical lesion coincides with her menses and resolves within four days with the completion of her menstrual period. Her menses are regular, occurring every 28–30 days and lasting for seven days. The initial four days are marked by heavy bleeding, clots, and significantly painful abdominal cramping, and the latter three days consist of light spotting.
A shave biopsy was performed at her dermatology visit which confirmed the diagnosis: umbilical endometriosis. She was referred to general surgery and underwent surgical excision of her umbilical endometriosis and primary closure of the fascial defect which successfully removed the lesion. Laparoscopy was offered to explore the abdominal cavity for peritoneal endometriosis, but the patient declined.
Following this diagnosis, the patient was also referred to OB/GYN for management of primary dysmenorrhea and endometriosis and started combined oral contraceptives. At OB/GYN follow-up one month later, the patient reported having a light, pain-free period and denied any further umbilical lesions or bleeding.
Discussion
Endometriosis is a benign condition involving the implantation of ectopic endometrial tissue outside of the uterus and has a prevalence of 6–11% in the United States [1]. While endometriosis most commonly manifests as shallow peritoneal implants, it may be found all over the abdominal cavity and can affect bladder, bowel, omentum, lung, heart, and even brain. In fact, 12% of cases of endometriosis present with extra-genital implants [2],[3]. Of these, umbilical endometriosis (UE), or Villar’s nodule, as described in 1886 by Villar, is the most common [4]. Given the overall rarity of the condition, awareness of UE is important for the primary care provider, gynecologist, or general surgeon who may be presented with patients with this condition first.
Umbilical endometriosis presents with an umbilical lesion located in the cutaneous or subcutaneous plane that is discolored brown, purple, or red due to bleeding [1],[4],[5]. Just as the endometrial lining of the uterus proliferates and sheds with the menstrual cycle, these ectopic endometrial implants also consist of functional tissue that are responsive to hormonal fluctuations [6]. This underlying mechanism accounts for why our patient noticed blood oozing from her umbilicus during her menses. Other than bleeding, the most commonly reported symptoms include pain and swelling of the nodule, and are most noticeable during menstruation [5].
Umbilical endometriosis generally appears in women of reproductive age; a systematic review by Dridi et al. reported a mean age of 37.9 years, with a range of 28.5 to 47.5. Comparatively, our 28-year-old patient is on the lower end of this age range, which may in part reflect the varying hormonal and environmental factors that are required for clinical presentation in different individuals. It is reported that about 33% of women with umbilical endometriosis have received a previous diagnosis of endometriosis [4],[5]. Our patient had not been previously diagnosed but complained of heavy bleeding and significant pain with menses that improved with hormonal contraceptive use, a clinical pattern consistent with the disease.
As our patient does not have any surgical history, this would be considered primary umbilical endometriosis [4],[5]. Primary UE represents almost 75% of all cases of UE and the mechanism behind its pathogenesis is vague. On the other hand, secondary umbilical endometriosis occurs much more clearly due to the seeding of surgical scars with uterine tissue following procedures such as episiotomy, cesarean section, and laparoscopy [7],[8]. Many theories have attempted to explain the pathogenesis of endometriosis and likewise UE. Embryonic remnants in the urachus and umbilical vessels may better explain cases of isolated umbilical endometriosis, wherein inflammation around the endometrial implant causes shedding and passage to the umbilicus via the umbilical venous system. More commonly, endometriosis has been explained via the theory of retrograde menstruation, wherein endometrial tissue flows backwards through the fallopian tubes during menstruation, seeding the abdominal cavity and presumably the umbilicus [5]. In fact, the prevalence of UE with co-existing pelvic implants is much higher than that of isolated UE, which lends more evidence to this theory [4].
There is a thought that UE travels via the same intra-abdominal currents initiated by large bowel peristalsis and respiratory movements that disseminate ovarian epithelial cells and Sister Mary Joseph nodules [4]. These malignancies can present similarly to UE. Differential diagnosis of an umbilical lesion also includes melanocytic nevus, incarceration of an umbilical hernia, pyogenic granuloma, urachal residual, and melanoma [2],[5],[9]. Our patient’s lesion was initially misdiagnosed as a skin tag and later a hemangioma before being biopsied.
While initial assessment is a clinical workup, the gold standard for diagnosis of cutaneous endometriosis requires biopsy. Histological diagnosis is made by the presence of two of the following features of either endometrial-like glands, endometrial stroma, or hemosiderin pigment [1],[5],[7],[10]. Cases with concomitant pelvic endometriosis may also have elevated levels of CEA and CA125 tumor markers. Ultrasound and magnetic resonance imaging (MRI) have been useful imaging techniques for characterizing and finding endometrial lesions. Umbilical nodules appear as a spherical finding within the dermal-epidermal layer with varied echogenicity on ultrasound. Magnetic resonance imaging in particular is helpful in studying deep pelvic endometriosis which show fibrous lesions with varied enhancement that are hypo or isointense on T1 and T2 [2].
The mean time from onset of symptoms to diagnosis and treatment has been reported to be 13.3 months. This delay in treatment is significant as the risk of future malignancy from UE has been reported to be about 3% [4],[9]. Thus, timely workup and biopsy is important for diagnosis and ruling out malignancy.
There is no standardized regimen for this condition since it is so rare [11]. The definitive management for umbilical endometriosis is surgical excision and repair of any disrupted local structures. Radical surgery with wide local excision is the preferred treatment and involves complete removal of the umbilicus and nodule whereas partial omphalectomy spares the umbilicus. Medical management alone with hormone analogues has not shown reliable results, perhaps due to lack of vascular accessibility and penetrance. However, pharmacotherapy (oral contraceptives, GnRH agonists/antagonists) may reduce endometrioma size. The literature reports that the recurrence rate of UE after surgical treatment is very low with no significant difference between radical or partial omphalectomy or with medical treatment [4],[5],[12]. Accordingly, a systematic review reported the effectiveness of surgical excision in 67.6% of patients [10].
Conclusion
This case demonstrates the rare case of a recurrent umbilical lesion in a young woman of reproductive age that was initially misdiagnosed. Recurrent dermatologic lesions or those in which the diagnosis is unclear should be followed up with a proper workup and biopsy in order to rule out malignancy. This case brings awareness to an overall rare condition and underlies the importance of keeping a broad differential and early referral services.
REFERENCES
1.
Moradi Y, Shams-Beyranvand M, Khateri S, Gharahjeh S, Tehrani S, Varse F, et al. A systematic review on the prevalence of endometriosis in women. Indian J Med Res 2021;154(3):446–54. [CrossRef]
[Pubmed]

2.
Sahli H, Boularab J, Mandour JE, Allali N, Chat L, Haddad SE. Primary umbilical endometriosis: Case report and literature review of an unusual cause of catamenial umbilical pain. Radiol Case Rep 2022;17(6):2133–6. [CrossRef]
[Pubmed]

3.
Chamié LP, Ribeiro DMFR, Tiferes DA, de Macedo Neto AC, Serafini PC. Atypical sites of deeply infiltrative endometriosis: Clinical characteristics and imaging findings. Radiographics 2018;38(1):309–28. [CrossRef]
[Pubmed]

4.
Dridi D, Chiaffarino F, Parazzini F, Donati A, Buggio L, Brambilla M, et al. Umbilical endometriosis: A systematic literature review and pathogenic theory proposal. J Clin Med 2022;11(4):995. [CrossRef]
[Pubmed]

5.
Capasso L, Sciascia V, Loiaco G, Guida G, Iarrobino F, Di Lillo C, et al. Primary subcutaneous umbilical endometriosis: Case report and review of the literature. Case Rep Surg 2020;2020:8899618. [CrossRef]
[Pubmed]

6.
Tsamantioti ES, Mahdy H. Endometriosis. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2025.
[Pubmed]

7.
Pramanik SR, Mondal S, Paul S, Joycerani D. Primary umbilical endometriosis: A rarity. J Hum Reprod Sci 2014;7(4):269–71. [CrossRef]
[Pubmed]

8.
Steck WD, Helwig EB. Tumors of the umbilicus. Cancer 1965;18:907–15. [CrossRef]
[Pubmed]

9.
Hirata T, Koga K, Kitade M, Fukuda S, Neriishi K, Taniguchi F, et al. A national survey of umbilical endometriosis in Japan. J Minim Invasive Gynecol 2020;27(1):80–7. [CrossRef]
[Pubmed]

10.
11.
Yao J, Zheng H, Nie H, Li CF, Zhang W, Wang JJ. Endometriosis of the lung: A case report and review of literature. World J Clin Cases 2023;11(18):4326–33. [CrossRef]
[Pubmed]

12.
Makena D, Obura T, Mutiso S, Oindi F. Umbilical endometriosis: A case series. J Med Case Rep 2020;14(1):142. [CrossRef]
[Pubmed]

SUPPORTING INFORMATION
Acknowledgments
We would like to thank the patient who graciously allowed us to share her story to bring attention to a rare presentation of a common gynecologic condition.
Author ContributionsJoyce Huang - Conception of the work, Design of the work, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Michelle Lu - Conception of the work, Design of the work, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Komal Soin - Conception of the work, Design of the work, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Guaranter of SubmissionThe corresponding author is the guarantor of submission.
Source of SupportNone
Consent StatementWritten informed consent was obtained from the patient for publication of this article.
Data AvailabilityAll relevant data are within the paper and its Supporting Information files.
Conflict of InterestAuthors declare no conflict of interest.
Copyright© 2025 Joyce Huang et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information.