|
Case Report
Unusual cervicothoracic presentation of lipoblastoma in a 12-month infant
1 MD, Resident in Radiology, Department of Radiology, Children's Hospital, UHC Ibn Sina, Rabat, Morocco
2 MD, Intern in Radiology, Department of Radiology, Children's Hospital, UHC Ibn Sina, Rabat, Morocco
3 Professor, Radiology, Department of Radiology, Children's Hospital, UHC Ibn Sina, Rabat, Morocco
4 Professor, Chief of Department of Radiology, Department of Radiology, Children's Hospital, UHC Ibn Sina, Rabat, Morocco
Address correspondence to:
El Mansoury Fatima Zahrae
Groupe Al Ahd, Hay Nahda 1, N° 1061, Rabat,
Morocco
Message to Corresponding Author
Article ID: 101291Z01EZ2022
Access full text article on other devices

Access PDF of article on other devices

How to cite this article
Zahrae EMF, Ismail HM, Najlae L, Nazik A, Latifa C. Unusual cervicothoracic presentation of lipoblastoma in a 12-month infant. Int J Case Rep Images 2022;13:101291Z01EZ2022.ABSTRACT
Introduction: Lipoblastomas (LBs) are infrequent tumors that typically manifest at the expense of embryonic adipocytes in infants younger than three years with a male predominance. Usually LBs are benign in nature, slow in growth with tendency to be localized in the extremities but it can also have an aggressively infiltrative tendency.
Case Report: We report a 1-year-old male child presented with painless cervicothoracic tumefaction investigated essentially with magnetic resonance imaging (MRI) which was characteristic of LBs, and further proved histologically. The child was managed surgically and the tumor was resected completely.
Conclusion: Lipoblastomas are extremely rare tumors that should figure in the differential diagnosis dealing with children presenting painless soft tissue mass that is growing. Magnetic resonance imaging findings are characteristics for the diagnosis which are confirmed by histopathological examination.
Keywords: Axilla, Cervicothoracic, Lipoblastoma, Magnetic resonance imaging
Introduction
Lipoblastoma (LB) is a highly rare tumor of soft tissue, only around 200 cases have been recorded so far worldwide [1]. It is a lipoid-based tumor and can present itself in two diametrically opposed benign forms: circumscribed or infiltrative which termed lipoblastomatosis [2]. Despite its benign biological behavior, its slow enlargement may cause compression to adjacent organs and structures resulting of several symptoms depending on the location [3]. Here, we present a case of an infant presenting with painless swelling of the neck as well as an abnormal growth within the axillary and thoracic area.
Case Report
A 1-year-old male child presented with painless tumefaction extending all the way from the first false rib to the base of the neck via the arm pit. The mass has progressively increased volume in the prior weeks .On clinical examination, diffuse cervicothoracic swelling was noted on the right side, which was compressible. No bruit or pulsations noted. No signs of inflammation were seen in the overlying skin. No sensitive nor motor deficit in the right arm was noted.
Magnetic resonance imaging (MRI) with gadolinium injection revealed a well-defined mass centered on the right lateral thoracic wall insinuating into the right axilla and extending to the deep inter muscular compartments of the base of the neck, measuring 5.7 × 7.5 × 12.9 cm .The lesion had predominant fat attenuation, with multiple fibrous septations and soft tissue nodules. On T1W1 sequence, these nodules were characterized by a mild contrast enhancement after gadolinium administration (Figure 1).
Topographically, the mass started from C6 vertebral level repelling the sternocleidomastoid muscle exteriorly and the cervical vascular package interiorly. The extended mass arrived into the right axillar area where the nervous brachial plexus was seen to drape around the mass (Figure 2A and Figure 2B). Up until the level of the 8th rib, we still noticed the mass effect on the chest wall in the form of inward bowing of the ribs but no intrathoracic extension. Imaging findings were characteristic of lipoblastoma, which was further proved histologically. The extension assessment did not find any metastatic location.
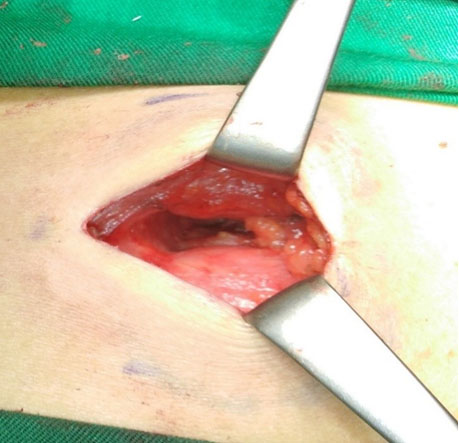
The child was managed surgically and during the surgical exploration, the tumor was completely encapsulated, it pushed back the vascular and nervous structures without any sign of invasion, it was resected completely.
Discussion
Ultrasound (US) is the first-line method of investigation, particularly in children. Characterized by a well-defined hyperechoic mass, with adipose component, accompanied with internal septations [1].
The Gold standard imaging method preferably chosen to diagnosis LB is the MRI. It usually present itself as a solid encapsulated mass with heterogeneous hyperintense signal in T1-weighted (Figure 1A and Figure 1B) and T2-weighted sequences due to its components or septations which consist mainly in fat and fibro-myxoid tissues has been noticed (Figure 1C and Figure 1D) [4],[5]. Usually the fat signal is less intense in T1-weighted sequences (Figure 1B). Naturally, the fat suppression sequence is particularly useful to confirm the presence of lipomatous features [6].
The main mimickers of the LB tumors are hibernoma, rare benign fatty tumor that arises from the fetal brown fat, and myxoid liposarcoma [4], which is rare in children younger than 10 years and has a well-described tendency to be aggressive; therefore it is important to exclude this diagnosis [6].
Recent statics that the preferred emerging sites of LB tumors are extremities by 27% followed by neck by 19%, then the gluteal region by 18%, then chest and the mesentery by 14%, lastly axilla 4% [5],[7]. In our case, the topography is centered around the axilla area which is the rarest location and the mass expended into the cervical area going up and the chest going down [1],[7]. The whereabouts of such LBs can come with clinical and management difficulties (Figure 2A and Figure 2B).
Clinically, these types of LBs can have significant growth, resulting in symptoms caused by mass effect [3] that include respiratory compromise (dyspnea and tracheal deviation) as of neurovascular encasement in the neck and superior mediastinum where tumor surrounded major vessels and nerves (Figure 2A and Figure 2B). A few cases of such neurovascular encasement have been reported in which LB surrounded but did not invade vessels wall [1],[7].
The intricacy and the intimate anatomical report of such tumors can be problematic at surgery because of the absence of discrete lesion features to discern margins intraoperatively [8]. Magnetic resonance imaging is uniquely suited, with its superior soft-tissue contrast, for delineating total lesion extent prior to resection and is essential in the evaluation of any deep LB [2],[6].
Although there is a high recurrence rate with incomplete resections, it depends on the extent of resection. If the tumor is completely resected, the prognosis is excellent, for instance in our case, it can be delicate to discern the surrounding of the tumor and how far the extension goes in some location such as the brachial plexus area (Figure 2). Chemotherapy is unnecessary in these patients [1],[7]. Post-surgery, a minimum of five years is essential for following-up in order to identify any recurrences [1]. Also, It has been described at least once in literature a case of spontaneous dissolvement of an LB in follow-up MRI, so a wait-and-see approach should be kept in mind in some cases [6].
Conclusion
In conclusion, cervicothoracic and axillar LB are extremely rare tumors that should figure in the differential diagnosis dealing with children with a painless head or neck soft tissue mass that is growing. Understanding their appearances is crucial in order to differentiate it from main mimickers, in particular liposarcoma. The definitive diagnosis is confirmed by histopathological examination, and surgery is usually the first-line treatment thus the pivotal role of accurately describing the topographic radiological extensions of the tumor according to nearby anatomical structures.
REFERENCES
1.
Séguier-Lipszyc E, Baazov A, Fichman S, Ash S, Freud E. Current management of lipoblastoma. Eur J Pediatr 2018;177(2):237–41. [CrossRef]
[Pubmed]

2.
Capasso R, Rossi E, Castelli L, et al. Mesenteric lipoblastoma and cervical lipoblastomatosis: Ultrasound, elastosonography, and computed tomography findings in two children. Case Rep Radiol 2014;2014:478252. [CrossRef]
[Pubmed]

3.
Aggarwal A, Goyal A, Kandasamy D. Lipoblastoma – A rare benign immature adipocytic neoplasm. Indian J Musculoskelet Radiol 2019;1(2):124–6. [CrossRef]

4.
Degnan AJ, Jelinek JS, Murphey MD. Lipoblastoma: Computed tomographic and magnetic resonance imaging features correlate with tumor behavior and pathology. Pediatr Radiol 2021;51(4):614–21. [CrossRef]
[Pubmed]

5.
Lomoro P, Simonetti I, Nanni AL, et al. Imaging of head and neck lipoblastoma: Case report and systematic review. J Ultrasound 2021;24(3):231–9. [CrossRef]
[Pubmed]

6.
Navarro OM. Pearls and pitfalls in the imaging of soft-tissue masses in children. Semin Ultrasound CT MR 2020;41(5):498–512. [CrossRef]
[Pubmed]

7.
Vo NH, Mashiana MK, Vo CC, Ward K, Nguyen J. Atypical presentation of lipoblastoma of a 9-month-old. Ear Nose Throat J 2019;98(5):261–2. [CrossRef]
[Pubmed]

8.
Chen CW, Chang WC, Lee HS, Ko KH, Chang CC, Huang GS. MRI features of lipoblastoma: Differentiating from other palpable lipomatous tumor in pediatric patients. Clin Imaging 2010;34(6):453–7. [CrossRef]
[Pubmed]

SUPPORTING INFORMATION
Author Contributions
El Mansoury Fatima Zahrae - Conception of the work, Design of the work, Acquisition of data, Analysis of data, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Halfi Mohamed Ismail - Analysis of data, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Lrhorfi Najlae - Analysis of data, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Allali Nazik - Analysis of data, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Chat Latifa - Conception of the work, Design of the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Guaranter of SubmissionThe corresponding author is the guarantor of submission.
Source of SupportNone
Consent StatementWritten informed consent was obtained from the patient for publication of this article.
Data AvailabilityAll relevant data are within the paper and its Supporting Information files.
Conflict of InterestAuthors declare no conflict of interest.
Copyright© 2022 El Mansoury Fatima Zahrae et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information.