|
Case Report
Salmonella osteomyelitis of calvarium: A rare infection and brief review
1 Senior Radiologist, Department of Radiology, Kasemrad Rattanathibeth General Hospital, Nonthaburi, Thailand
2 Neurosurgeon interventionist Neuro, Department of Surgery, Bhumipol Adulyadej Hospital, Royal Thai Air Force, Bangkok, Thailand
Address correspondence to:
Utit Pitaktong
MD, FICS, 69/273 Mu 12, Puttamonton Sai 3 Soi 21 Road, Salathammasop, Taweewattana, Bangkok 10170, Thailand; Kasemrad Rattanathibeth General Hospital, 58 M.15, Rattanathibeth Road, Bangrakpattana, Bangbuathong, Nonthaburi 11110,
Thailand
Message to Corresponding Author
Article ID: 101506Z01UP2025
Access full text article on other devices

Access PDF of article on other devices

How to cite this article
Pitaktong U, Thanyanopporn J. Salmonella osteomyelitis of calvarium: A rare infection and brief review. Int J Case Rep Images 2025;16(1):95–100.ABSTRACT
Salmonella species are the cause of enteric fever in humans, presenting with fever and gastrointestinal symptoms such as diarrhea or constipation. Bacteremia is another form of this infection. The organism can be harbored in the body for years, and disseminated to other organs, especially in patients with preexisting conditions such as hemoglobinopathies, diabetes mellitus, previous joint trauma or surgery, connective tissue disease, or even immunocompetent person without predisposing factors. Salmonella osteomyelitis is a rare sequalae of salmonellosis caused by blood stream spreading of the organism. Salmonellosis of the skull is extremely rare, with only 15 reported cases in the literatures up to date. We report a case of salmonella osteomyelitis of the skull from a secondary hospital in Bangkok, Thailand.
Keywords: Calvarium osteomyelitis, Metastatic abscess, Osteomyelitis, Salmonella osteomyelitis, Salmonellosis
Introduction
Salmonellosis can present in almost any sites of the body including the bones and the brain [1]. Osteomyelitis is primarily caused by Staphylococcus aureus and Staphylococcus epidermidis which are the common skin floras. Osteomyelitis caused by Salmonella spp. infection is rare, accounted for only 0.8% of all salmonella infections [2], and 0.45% of all the osteomyelitis cases [3]. Most cases result from hematogenous seeding during bacteremia [1],[4],[5],[6],[7].
Salmonella osteomyelitis of the calvarium is extremely rare, with only 15 cases that have been reported up to date. Most of them were caused by Salmonella (S) typhi, only three by S. paratyphi A and B. We report a case of salmonella osteomyelitis of calvarium with underlying connective tissue disease (systemic lupus erythematosus, SLE) and history of several episodes of diarrhea in the past.
Case Report
A female in early 60s with SLE was presented to Kasemrad Rattanathibeth Hospital located in Bangkok, Thailand, with a painless scalp mass at the vertex. Her next of kin reported of the patient’s three-month diarrhea with vomiting. On examination, the patient displayed a 6-cm scalp mass at the vertex without tenderness and with normal consciousness. The initial complete blood count (CBC) on Day 1 was 11.70 cell/µL (normal range=4.4–11.3 cell/µL) with neuthrophils 77%. The erythrocyte sediment rate (ESR) was 91 mm/h (normal < 20 mm/h). Blood cultures were done and showed the result as Salmonella spp. Computed tomography (CT) scans showed an osteolytic lesion at the mid line epidural space without brain involvement (Figure 1 and Figure 2). Magnetic resonance (MR) images in sagittal view show a lesion with bone loss and thin-walled cystic nature without contrast enhancement (Figure 3 and Figure 4). The dura is intact and shows fluid–fluid level (Figure 5), with no periosteal reaction. Findings indicate that this is an extradural thin-walled cystic lesion with fluid content in different consistency caused by benign chronic process which causes bone loss.
Intravenous antibiotics was started immediately with combination of piperacillin and tazobactam since Day 1 to the last day of admission (Day 15). Intravenous ceftriaxone was added from Day 9 to Day 15. She was scheduled for craniotomy and mass removal on Day 4. The CBC declined to be 5.1 cell/µL, neuthrophils 81% on Day 14. The ESR was 17 mm/h on Day 9.
During the operation, special attention was paid to avoid dural injury by carefully respecting the granulation tissue and dura matter for, in a dural abscess, dural tear would cause potentially severe consequences like meningitis. Removal of tissue debris and bone erosion in operative field were also performed. The pathologic report of the bone specimen from vertex of the skull indicated chronic and acute osteomyelitis without abscess formation, and no granuloma or neoplastic lesions.
Two weeks after the surgery, pus penetrated through the center of the wound. Pus cultures confirmed Salmonella species (spp.) without drug resistance. On Day 15, CBC was now 5.3 cell/µL and ESR rose to 74 mm/h, implying progression of the infection.
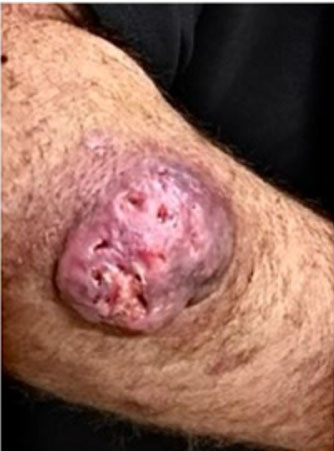
Six weeks after intravenous antibiotics, metastatic pus appeared on the forehead measuring 7 cm. Re-cultures confirmed a Salmonella spp. infection. Finally, three months after the surgery, the patient developed clinical signs of unconsciousness with high fever. Hemoculture results indicated Salmonellosis septicemia. Unfortunately, the patient died days later from salmonella septicemia.
Discussion
Salmonella is a gram-negative bacillus that can cause various human infections like gastroenteritis, enteric fever, bacteremia, vascular infection, focal infection, and an asymptomatic chronic carrier [1],[2],[5] [6],[7],[8]. Enteric fever usually presents as acute febrile illness and headache, diarrhea or constipation, bradycardia, splenomegaly and leukopenia, and, rarely, involving skeletal, cardiovascular, pulmonary, hepatobiliary, genitourinary, and central nervous systems [4],[9]. Only 67 cases of salmonella osteomyelitis have been published from 1970 to 2019 [2], mostly affecting ribs, spine [10],[11] and long bones [10],[12],[13], and occasionally skull but rare [14]. Up to date, there are only 15 reported cases [14],[15] with preference for adults to children. Men and women are equally affected.
Predisposing conditions for salmonella osteomyelitis include hemoglobinopathies (e.g., sickle-cell disease), diabetes mellitus, connective tissue disease (e.g., systemic lupus erythematosus), corticosteroid therapy, lymphoma, liver and cardiovascular disease, previous surgery or trauma, and travel to endemic areas or countries [16]. Immunocompetent adults who are absent common risk factors for salmonella osteomyelitis can get the disease as well [2],[3],[4].
The common manifestations of the skull osteomyelitis are fever, headache, seizure and focal neurological signs, or local swelling [17]. Few patients have diarrhea or recent history of diarrhea due to long incubation periods and non-intestinal entry routes of infection [2]. In some cases, there is a considerable delay between the development of skeletal osteomyelitis and the initial illness with typhoid fever ranging from 33 to 47 years [10],[18], reflecting the stage of chronic carriers of the salmonella organism. This could potentially be due to insufficient treatment given for enteric fever leading to subsiding of the symptoms but not a complete cure and subsequently persisting infections [4].
Besides the initial conventional laboratory tests and imaging procedures like radiography which usually are nonspecific, cultures from aspiration or biopsy are valuable for definite diagnosis as they were positive for all Salmonella osteomyelitis patients [2]. Imaging examinations are very helpful for the diagnosis and demonstration of the lesion(s). Radiography will show changes that are of the usual osteomyelitis, i.e., central area of radiolucency of damaged bone with a surrounding thick rim of reactive bone sclerosis, and variable degree of periosteal new-bone formation [19]. Computed tomography (CT) images will show bone erosion or destruction accompanied by thickening of the dura in the region of complete bone loss, and thinning of the overlying skin . Magnetic resonance (MR) images will show bone marrow edema (decreased T1 signal and increased T2 signal), periosteal and dural enhancement, adjacent soft tissue inflammation, and osteolytic lesions [20].
Treatment consists of combinations of prolonged antibiotics therapy and surgery for cases with intracranial or brain involvement. Six to 8 weeks of antibiotics therapy will achieve favorable results. At least 2-month therapy for uncomplicated cases and a 3-month course for chronic or complicated infections are suggested [21],[22]. Third-generation cephalosporins are the most common agents of choice [23]. However, resistance to third-generation cephalosporins has also been reported [21],[24]. Fluoroquinolone which once was used for treatment of salmonella osteomyelitis are failing because resistance has become increasingly common [25].
In cases of local swelling with bone involvement, radical debridement of the lesion is recommended [26]. For cases of brain abscesses or initial collection, complete drainage is necessary. Surgical intervention in the management of salmonella osteomyelitis may include craniotomy, removal of damaged bone, drainage and removal of extradural pus and granulation tissue [27].
Our case presented as an epidural abscess which was proved to be salmonellosis by pus cultures. Despite six weeks of antibiotics treatment, the patient developed a metastatic abscess at the forehead that was salmonella infection as evidenced by pus cultures. The patient returned to the hospital again Three months after the surgery with signs and symptoms of salmonella septicemia proved by blood cultures; the silent stage of bacteremia was implied. Unfortunately, she died a few days later from Salmonella septicemia.
Conclusion
Salmonella osteomyelitis is an uncommon disease but should be considered by clinicians when evaluating osteomyelitis cases. Awareness of its potential occurrence even in immunocompetent individuals is essential for timely diagnosis and management. Salmonella osteomyelitis of the skull is a rare condition. Anticipated consideration in patients with focal swelling on the head is important. Cranial imaging procedures with contrast agents CT or MRI should be performed. Prolonged antibiotics therapy is necessary. In case of intracranial extension, surgical treatment should be extensive enough to exclude any underlying intracranial abscess in addition to the prolonged antibiotics therapy.
REFERENCES
1.
Cohen JI, Bartlett JA, Corey GR. Extra-intestinal manifestations of salmonella infections. Medicine (Baltimore) 1987;66(5):349–88. [CrossRef]
[Pubmed]

2.
Huang ZD, Wang CX, Shi TB, et al. Salmonella osteomyelitis in adults: A systematic review. Orthop Surg 2021;13(4):1135–40. [CrossRef]
[Pubmed]

3.
Arora A, Singh S, Aggarwal A, Aggarwal PK. Salmonella osteomyelitis in an otherwise healthy adult male-successful management with conservative treatment: A case report. J Orthop Surg (Hong Kong) 2003;11(2):217–20. [CrossRef]
[Pubmed]

4.
Rohilla R, Bhatia M, Gupta P, Singh A, Shankar R, Omar BJ. Salmonella osteomyelitis: A rare extraintestinal manifestation of an endemic pathogen. J Lab Physicians 2019;11(2):164–70. [CrossRef]
[Pubmed]

5.
Reddy MP, Sulaiman ZI, Askar G. Vertebral discitis caused by Salmonella enterica serovar Montevideo infection. IDCases 2023;33:e01882. [CrossRef]
[Pubmed]

6.
7.
Toofan Y, Tarun S, Bender JD, Auerbach SA, Stewart DA, Watson ME Jr. Vertebral osteomyelitis due to Salmonella Poona in a healthy adolescent female. SAGE Open Med Case Rep 2020;8:2050313X20969017. [CrossRef]
[Pubmed]

8.
Banky JP, Ostergaard L, Spelman D. Chronic relapsing Salmonella osteomyelitis in an immunocompetent patient: Case report and literature review. J Infect 2002;44(1):44–7. [CrossRef]
[Pubmed]

9.
Huang DB, DuPont HL. Problem pathogens: Extra-intestinal complications of Salmonella enterica serotype Typhi infection. Lancet Infect Dis 2005;5(6):341–8. [CrossRef]
[Pubmed]

10.
Hurt W, Stephenson J, Hutchinson J, Godbole G, Chattaway MA. A rare case of Salmonella Paratyphi C osteomyelitis: A genetic analysis and review of Salmonella osteomyelitis in England. Diagn Microbiol Infect Dis 2023;105(3):115877. [CrossRef]
[Pubmed]

11.
Saravu K, Bhat SN, Gupta N. Spondylodiscitis due to Salmonella Typhi: A series of four cases. Oxf Med Case Reports 2021;2021(11–2):omab128. [CrossRef]
[Pubmed]

12.
Hamada T Sr, Furukawa S, Kikuchi Y, Kubota M, Mitsunaga E. An atypical case of spondylitis due to nontyphoidal salmonella in an adult patient: A case report and review of the literature. Cureus 2024;16(2):e55034 [CrossRef]
[Pubmed]

13.
Rentmeister V, Lorenzo-Villalba N, Gorur Y, Yerna M, Ali D. Salmonella osteomyelitis of unknown origin: An underestimated infection. Eur J Case Rep Intern Med 2023;10(11):004092. [CrossRef]
[Pubmed]

14.
Warade AC, Agrawal US, Sunawala AJ, Desai K. Salmonella osteomyelitis of skull bone: A rare case. Neurol India 2021;69(4):1070–1. [CrossRef]
[Pubmed]

15.
Rodriguez RE, Valero V, Watanakunakorn C. Salmonella focal intracranial infections: Review of the world literature (1884–1984) and report of an unusual case. Rev Infect Dis 1986;8(1):31–41. [CrossRef]
[Pubmed]

16.
Klochko A, Bronze MS. Salmonella infection (salmonellosis). [Available at: https://emedicine.medscape.com/article/228174-print]

17.
Bullitt E, Lehman RA. Osteomyelitis of the skull. Surg Neurol 1979;11(3):163–6.
[Pubmed]

18.
Herbert DA, Ruskin J. Salmonella typhi epidural abscess occurring 47 years after typhoid fever. Case report. J Neurosurg 1982;57(5):719–21. [CrossRef]
[Pubmed]

19.
Gaillard F, Glick Y, Verikios N, et al. Osteomyelitis. Reference article, Radiopaedia.org (Accessed on 24 May 2025). [Available at: https://radiopaedia.org/articles/7662]

20.
Hartung M, Chronic osteomyelitis – calvarial (severe). Case study, Radiopaedia.org (Accessed on 24 May 2025). [Available at: https://radiopaedia.org/cases/69668]

21.
Lamichhane B, Mawad AMM, Saleh M, et al. Salmonellosis: An overview of epidemiology, pathogenesis, and innovative approaches to mitigate the antimicrobial resistant infections. Antibiotics (Basel) 2024;13(1):76. [CrossRef]
[Pubmed]

22.
Santos EM, Sapico FL. Vertebral osteomyelitis due to salmonellae: Report of two cases and review. Clin Infect Dis 1998;27(2):287–95. [CrossRef]
[Pubmed]

23.
24.
Saha SK, Talukder SY, Islam M, Saha S. A highly ceftriaxone-resistant Salmonella typhi in Bangladesh. Pediatr Infect Dis J 1999;18(4):387. [CrossRef]
[Pubmed]

25.
Cotter L, Mushtaq M, Gonzalez A. A case of vertebral osteomyelitis due to quinolone-resistant Salmonella paratyphi A. BMJ Case Rep. 2009;2009:bcr07.2008.0400. [CrossRef]
[Pubmed]

26.
Sanchez AA, Mazurek MT, Clapper MF. Salmonella osteomyelitis presenting as fibrous dysplasia. A case report. Clin Orthop Relat Res 1996;(330):185–9. [CrossRef]
[Pubmed]

27.
Thakur K, Singh DV, Goel A. Cranial vault Salmonella osteomyelitis leading to extradural abscess – A case report. Indian J Med Microbiol 2002;20(4):219–20.
[Pubmed]

SUPPORTING INFORMATION
Author Contributions
Utit Pitaktong - Conception of the work, Design of the work, Acquisition of data, Analysis of data, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Jackree Thanyanopporn - Acquisition of data, Analysis of data, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Guaranter of SubmissionThe corresponding author is the guarantor of submission.
Source of SupportNone
Consent StatementWritten informed consent was obtained from the patient for publication of this article.
Data AvailabilityAll relevant data are within the paper and its Supporting Information files.
Conflict of InterestAuthors declare no conflict of interest.
Copyright© 2025 Utit Pitaktong et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information.