|
Case Report
Case report: Rare case of spontaneous and non-traumatic vulvar epidermoid cyst
1 Assistant Professor, Radiology Department, Aga Khan University Hospital, Karachi, Sindh, Pakistan
2 Specialist Radiologist, Radiology Department, Bahrain Specialist Hospital, Al Juffair, Manama, Bahrain
3 Consultant Radiologist, Radiology Department, Jinnah Postgraduate Medical Center, Karachi, Sindh, Pakistan
4 Radiology Resident, Radiology Department, Aga Khan University Hospital, Karachi, Sindh, Pakistan
5 Women Imaging Fellow, Radiology Department, Aga Khan University Hospital, Karachi, Sindh, Pakistan
Address correspondence to:
Fatima Qaiser
Aga Khan University Hospital, Stadium Road, Karachi, Sindh,
Pakistan
Message to Corresponding Author
Article ID: 100208Z08GS2025
Access full text article on other devices

Access PDF of article on other devices

How to cite this article
Shafqat G, Shaikh A, Kaleemi R, Ahmed M, Qaiser F. Case report: Rare case of spontaneous and non-traumatic vulvar epidermoid cyst. J Case Rep Images Obstet Gynecol 2025;11(1):97–101.ABSTRACT
Introduction: Epidermoid cysts are nodular structures lined with stratified squamous epithelium. In most cases, epidermoid cysts arise in the head and neck region, or in extremities, with their occurrence in the female genital tract being rare. Cases of epidermoid cysts in the female genital tract tend to have a history of trauma—mostly surgical or due to female genital tract mutilation. We present a case of biopsy proven vulvar epidermoid cyst which arose without a background of prior surgical history, female genital mutilation, or other trauma.
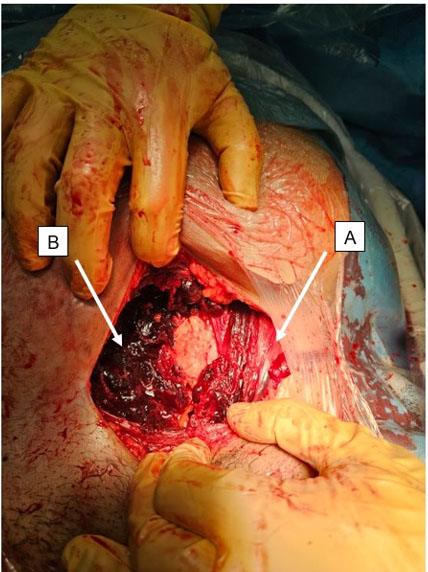
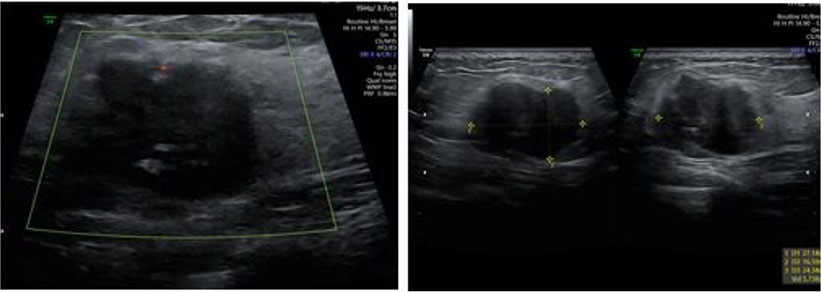
Case Report: A 25-year-old multigravida female with two children presented with progressive painless vulvar swelling for around two years, without any history of trauma or prior surgery. Vulvar ultrasound examination revealed a well-circumscribed, ovoid subcutaneous tissue mass arising from the labia majora with internal linear echogenic and anechoic foci, as well as raised through-transmission. Magnetic resonance imaging (MRI) examination revealed an exophytic, round-to-ovoid subcutaneous mass lesion in the vulvar region which returned iso- to hyperintense signals on T1, hyperintense signals on T2-weighted images, and hyperintense signals on diffusion weighted imaging (DWI), while demonstrating a peripheral rim of enhancement on T1 post-contrast images. The patient underwent surgical excision without any complications and histopathology reaffirmed the diagnosis of vulvar epidermoid cyst having a stratified squamous epithelial lining.
Conclusion: While epidermoid cysts of the female genital tract are rare occurrences in patients lacking prior surgical or traumatic history, they need to be considered as possible differential diagnoses in patients presenting with characteristic symptoms and imaging findings. Further evaluation of the clinical course and imaging findings of epidermoid cysts in the female genital tract, as well as the efficacy of different imaging modalities and interventions is essential to improve their diagnosis and management.
Keywords: Epidermoid cyst, Female genital tract, Non-traumatic, Vulvar lesion
SUPPORTING INFORMATION
Author Contributions
Gulnaz Shafqat - Substantial contributions to conception and design, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published
Asra Shaikh - Substantial contributions to conception and design, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published
Raima Kaleemi - Revising it critically for important intellectual content, Final approval of the version to be published
Mudassir Ahmed - Revising it critically for important intellectual content, Final approval of the version to be published
Fatima Qaiser - Revising it critically for important intellectual content, Final approval of the version to be published
Guaranter of SubmissionThe corresponding author is the guarantor of submission.
Source of SupportNone
Consent StatementWritten informed consent was obtained from the patient for publication of this article.
Data AvailabilityAll relevant data are within the paper and its Supporting Information files.
Conflict of InterestAuthors declare no conflict of interest.
Copyright© 2025 Gulnaz Shafqat et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information.