|
Case Report
Obstructed hemivagina and ipsilateral renal anomaly (OHVIRA) syndrome: A case report
1 Senior House Officer, Accident and Emergency Department, Queen Elizabeth Hospital, Barbados
Address correspondence to:
Keturah Murray
Senior House Officer, Accident and Emergency Department, Queen Elizabeth Hospital
Barbados
Message to Corresponding Author
Article ID: 100175Z08KM2024
Access full text article on other devices

Access PDF of article on other devices

How to cite this article
Murray K. Obstructed hemivagina and ipsilateral renal anomaly (OHVIRA) syndrome: A case report. J Case Rep Images Obstet Gynecol 2024;10(2):1–5.ABSTRACT
Obstructed hemivagina and ipsilateral renal anomaly (OHVIRA) syndrome is a rare congenital abnormality marked by a triad of uterine didelphys, obstructed hemivagina, and ipsilateral renal anomaly. The condition is asymptomatic in the pre-pubertal females. Commonly it is diagnosed in young females, within a year of menarche, who present with cyclical pelvic pain with or without a mass. Rarely, these patients are identified later in life, many years after initiation of menses, and a high clinical index of suspicion must be kept. Presented here is a case of OHVIRA syndrome diagnosed in a 22-year-old nulliparous female who presented to the Accident and Emergency Department (AED) of the Queen Elizabeth Hospital, Barbados, with a two-month history of abdominal pain. A laparotomy with right ovarian cystectomy and vaginal incision and drainage of left hematocolpos with marsupialization was performed and the patient was discharged with no complications.
Keywords: Laparotomy, Müllerian anomaly, OHVIRA syndrome
Introduction
Formerly known as Herlyn–Werner–Wunderlich syndrome, OHVIRA syndrome was first reported in 1922. It can represent a diagnostic challenge due its rarity and heterogenous presentation [1],[2]. Imaging modalities such as ultrasound (US) are useful; however, currently the gold standard investigation is with magnetic resonance imaging (MRI). The mainstay of management is surgical relief of the obstructed hemivagina; delays in diagnoses can be associated with the development of pelvic inflammatory disease (PID), endometriosis, and pelvic adhesions [3]. Thus, prompt diagnosis and intervention are paramount in the successful management of these patients.
Case Report
A 22-year-old nulliparous female presented to the Accident and Emergency Department (AED) of the Queen Elizabeth Hospital, Barbados, on February 7th, 2024, with a two-month history of episodes of sharp, constant, non-radiating, and severe right lower quadrant pain which worsened two days prior to presentation. This was associated with a one-day history of subjective fever, decreased appetite, and a history of yellow-brown discharge per vaginum. Her last reported sexual intercourse with one month prior with a male partner; no barrier methods of protection were used.
Her menarche was at 11 years old which was initially painful then heavy for “a few months.” She had been amenorrheic for three years due to medications started by her physician, then noted a spontaneous return of menses occurring twice per month. She denied dyspareunia, dyschezia, or dysuria.
The patient was seen in the AED two weeks prior and was diagnosed with pelvic inflammatory disease (PID) and discharged to complete a fourteen-day course of doxycycline 100 mg twice a day (bd) and metronidazole 500 mg (bd) with a gynecology ward review in two days. However, due to worsening of the abdominal pain, despite completing the antibiotic regimen prescribed, she decided to re-present to the AED for further evaluation.
Her vital signs at presentation were normal; blood pressure of 124/81 mmHg, pulse 75 beats per minute (bpm), temperature 36.4 °C, and oxygen saturations of 99% on room air.
Her abdomen was soft and non-distended. There was significant right lower quadrant tenderness with guarding, but no rebound. On vaginal examination, there was extreme right adnexal tenderness. There were no internal masses palpated, a single cervix was visualized; this was normal.
A complete blood count, urea, and electrolytes and cardiac enzymes were normal, and her 12-lead electrocardiogram showed a normal sinus rhythm at 72 bpm. Her urine pregnancy test was negative.
At this point differential diagnoses included complications of PID such as pyosalpinx and tubo-ovarian abscess and given the sub-acute worsening of her symptoms, a diagnosis of acute appendicitis needed to be further investigated. Therefore, the decision was made to perform urgent computed tomography (CT) of the abdomen and pelvis with contrast (Figure 1 and Box 1).
The patient was subsequently admitted to the gynecology ward where an ultrasound (US) scan performed by a senior registrar of the obstetrics and gynecology department showed uterine didelphys with a left hematocolpos and a simple ovarian cyst (Box 2).
The decision was made to proceed with surgical management. A laparotomy with right ovarian cystectomy and vaginal incision and drainage of left hematocolpos with marsupialization was performed.
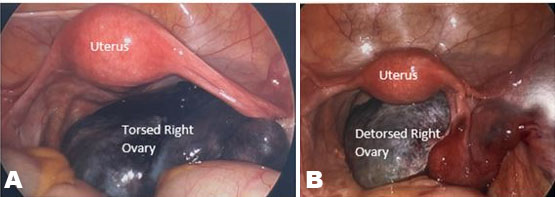
Under general anesthesia, her abdomen was opened using a Pfannenstiel incision. Intraoperative findings were:
- A heart shaped uterus approximately 6 cm width, 6 cm height, and 3 cm in diameter.
- Normal left ovary and normal fallopian tubes.
- Right ovary enlarged with a simple cyst.
- Endometriotic deposits to the right ovarian fossa and right posterior uterus.
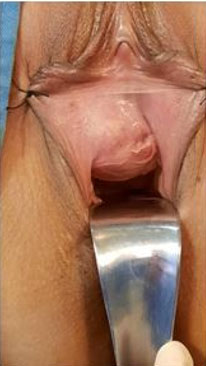
An attempt was made to dissect the cyst using blunt dissection; however, the cyst ruptured draining straw colored fluid. The cyst wall was then excised with blunt dissection. Hemostasis was achieved with cautery to the ovarian bed and the ovary closed with 3-0 vicryl (polyglactin 910). Peritoneal lavage was clear. An intraoperative digital exam performed revealed a bulge in the left upper vagina which was confirmed on speculum examination and dark red blood was seen coming from the os (one cervix seen).
A longitudinal incision was made to the upper left vagina approximately 7 cm from the introitus; pus and blood returned. A two-step marsupialization was done; 2-0 vicryl (polyglactin 910) sutures to the edges and angles then continuous sutures. Hemostasis was achieved and a vaginal pack left in place.
The patient had an uneventful postoperative period. The vaginal pack was removed the next day, and she was discharged on postoperative day three. Her histopathology report confirmed a follicular cyst (Box 3). She was discharged with a six week follow-up to the gynecology clinic. She was well and had no complications at this visit.
Discussion
The pathogenesis of OHVIRA syndrome is not completely understood. It is proposed to be associated with Müllerian duct abnormalities. The true incidence of congenital uterine anomalies is difficult to determine. Müllerian malformations have an estimated incidence of 1–3% in the general population. Obstructed hemivagina and ipsilateral renal anomaly has an incidence of 0.16–10% of these Müllerian duct anomalies [1].
Obstructed hemivagina and ipsilateral renal anomaly syndrome is the result of an embryological arrest of the Müllerian and mesonephric ducts at eight weeks of gestation [4]. Renal agenesis is the most common associated non-genital anomaly and is always seen on the side with the obstructed hemivagina [5]. Uterine didelphys, another feature of the syndrome, is classified by the American Fertility Society, as a Class 3, non-fusion anomaly. These occur due to an arrest during the second stage of embryologic development where the two separate Müllerian ductal systems fuse in the midline. This can begin at any level and can be incomplete [6]. To date, there have been no documented case reports of OHVIRA syndrome in Barbados.
Our patient was diagnosed ten years after menarche; however, OHVIRA syndrome is typically diagnosed shortly after menarche, on average, two months to one year [7]. These patients present with cyclic, increasing lower abdominal pain secondary to the hematocolpos present due to obstructed hemivagina [8]. Normal menstrual flow through the unobstructed hemivagina and symptoms resembling dysmenorrhea, which is common in this age group, can preclude an earlier diagnosis if suspicion is not high [8]. Albeit rarely, but as seen in our case, patients may present with abnormal vaginal discharge, acute abdominal pain, and fever [9]. Acute urinary retention in younger patients is another infrequent presentation [10] and there have also been documented cases diagnosed in the prenatal and newborn period due to renal agenesis or mucocolpos or hydrocolpos [8].
Magnetic resonance imaging (MRI) was not available at this institution; however, structural abnormalities were detected on both CT and US. An abdomen/pelvis CT scan is usually readily available in most units; however, it cannot depict the vagina as accurately as an MRI, and it exposes patients to radiation [3]. Ultrasound and MRI are widely and effectively used in the diagnosis of genitourinary anomalies, with close to 100% accuracy being reported for MRI [9]. While US is a widely available, non-invasive modality that is helpful in the detection of hematocolpos [8], MRI remains the gold standard for diagnosis due to its higher sensitivity in detecting the uterine morphology and the continuity of the vagina when compared to ultrasonography [8].
Many Müllerian duct anomalies do not require treatment. However, surgery is necessary for OHVIRA syndrome as soon as it is diagnosed to prevent long-term complications. The surgical management of these cases involves drainage of fluid and resection of the vaginal septum with great care to avoid compromise to the bladder, rectum, and the cervixes. The two cervixes may be at different levels and the tissue between them should be left in place so as not to compromise their blood supply [1]. Dissection of the septum can be a pure vaginal or a hysteroscopic approach but with the advancement of minimally invasive surgery, laparoscopy has started to gain interest in the management of such cases. This holds especially true in cases where a small hematocolpos is present, rendering a pure vaginal approach difficult as it is unable to well define the landmark for septum resection [11].
Sleiman et al. described the use of laparoscopy in the management of OHVIRA syndrome with a high vaginal septum, in order to avoid laparotomy in a patient whose family refused the transvaginal approach [12]. A skilled laparoscopic surgeon can use a minimal invasive approach as a safe alternative to laparotomy with better outcomes, such as a reduction in the postoperative pain and cosmetic injury, early ambulation, shorter hospital stay, and a rapid return to normal activities [12].
Intraoperatively, right ovarian endometriotic deposits were found for our patient. Endometriosis, in the form of ovarian or deep infiltrating endometriosis, is found in 17–36% of these patients, with the most likely pathogenesis being the inability of the obstructed hemivagina to distend due to the thick septum resulting in retrograde menstruation. Delayed diagnosis is associated with high rates of PID, pelvic adhesions, and endometriosis [3]. Common complications of surgery include dyspareunia, re-obstruction, and vaginal stenosis, though these vary dependent upon the type of surgery performed. For example, complete excision of the septal tissue may lead to circumferential scar formation and vaginal stenosis or a limited resection to create a window to drain the collected blood is more likely to be complicated by re-obstruction [1].
Concerning fertility, the pregnancy rate in women with uterine didelphys is reduced [13]. In up to 80% of cases, pregnancies are on the contralateral side of the obstructed hemivagina, but they have also been reported on the same side. High rates of preeclampsia (14%), preterm delivery (36%), breech presentation (38%), and a high cesarean section rate (67%) are common obstetric complications found in patients with OHVIRA syndrome, and the patients should be appropriately counselled [3]. Postoperatively, patients should also be followed up closely for the development of any renal or gynecological issues.
Conclusion
Obstructed hemivagina and ipsilateral renal anomaly syndrome is a rare congenital abnormality which is usually identified in young females shortly after menarche. One must, however, keep in mind that this syndrome can present later in life as early detection and prompt intervention are crucial to preventing the development of long-term complications.
REFERENCES
1.
Tug N, Sargin MA, Çelik A, Alp T, Yenidede I. Treatment of virgin OHVIRA syndrome with haematometrocolpos by complete incision of vaginal septum without hymenotomy. J Clin Diagn Res 2015;9(11):QD15–6. [CrossRef]
[Pubmed]

2.
Shah DK, Laufer MR. Obstructed hemivagina and ipsilateral renal anomaly (OHVIRA) syndrome with a single uterus. Fertil Steril 2011;96(1):e39–41. [CrossRef]
[Pubmed]

3.
Grammatis AL, Ajibade F, Warakaulle D, Dada T. Obstructed hemi-vagina with ipsilateral renal agenesis syndrome in adulthood: A diagnostic challenge. Diagnostics (Basel) 2023;13(21):3377. [CrossRef]
[Pubmed]

4.
Sharma R, Mishra P, Seth S, Argarwal N. OHVIRA syndrome—diagnostic dilemmas and review of literature. J South Asian Feder Obst Gynae 2020;12(6):421–6. [CrossRef]

5.
Jia G, Chai W, Cui M, Wen Y, Cui L, Gong F. A case report on Herlyn-Werner-Wunderlich syndrome with spontaneous abortion. Medicine (Baltimore) 2018;97(36):e12004. [CrossRef]
[Pubmed]

6.
Robbins JB, Broadwell C, Chow LC, Parry JP, Sadowski EA. Müllerian duct anomalies: Embryological development, classification, and MRI assessment. J Magn Reson Imaging 2015;41(1):1–12. [CrossRef]
[Pubmed]

7.
Orazi C, Lucchetti MC, Schingo PM, Marchetti P, Ferro F. Herlyn-Werner-Wunderlich syndrome: Uterus didelphys, blind hemivagina and ipsilateral renal agenesis. Sonographic and MR findings in 11 cases. Pediatr Radiol 2007;37(7):657–65. [CrossRef]
[Pubmed]

8.
Gungor Ugurlucan F, Bastu E, Gulsen G, Kurek Eken M, Akhan SE. OHVIRA syndrome presenting with acute abdomen: A case report and review of the literature. Clin Imaging 2014;38(3):357–9. [CrossRef]
[Pubmed]

9.
Mandava A, Prabhakar RR, Smitha S. OHVIRA syndrome (obstructed hemivagina and ipsilateral renal anomaly) with uterus didelphys, an unusual presentation. J Pediatr Adolesc Gynecol 2012;25(2):e23–5. [CrossRef]
[Pubmed]

10.
Adams GW Jr, Wilson CE, Holloway JH, Williamson HF. Uterus didelphys with unilateral imperforate vagina: A rare cause of acute urinary retention. J Urol 1979;121(1):131–2. [CrossRef]
[Pubmed]

11.
Moufawad G, Ayed A, Sleiman Z. Reconsidering the best minimally invasive approach for patients with Herlyn-Werner-Wunderlich syndrome: Should we push the frontiers for a better outcome? Front Surg 2023;10:1158753. [CrossRef]
[Pubmed]

12.
Sleiman Z, Wehbe GS, Rassy EE, et al. A novel surgical intervention for an uncommon entity: Laparoscopy-assisted resection of a vaginal septum in obstructed hemivagina and ipsilateral renal anomaly syndrome. J Laparoendosc Adv Surg Tech A 2019;29(5):714–6. [CrossRef]
[Pubmed]

13.
Tangshewinsirikul C, Dulyaphat W, Diawtipsukon S, Tingthanatikul Y, Satirapod C, Wattanasirichaigoon D. Successful pregnancy outcome in Herlyn-Werner-Wunderlich syndrome with pyocolpos: A case report and literature review. Clin Case Rep 2020;8(11):2217–22. [CrossRef]
[Pubmed]

SUPPORTING INFORMATION
Author Contributions
Keturah Murray - Conception of the work, Design of the work, Acquisition of data, Analysis of data, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Guaranter of SubmissionThe corresponding author is the guarantor of submission.
Source of SupportNone
Consent StatementWritten informed consent was obtained from the patient for publication of this article.
Data AvailabilityAll relevant data are within the paper and its Supporting Information files.
Conflict of InterestAuthor declares no conflict of interest.
Copyright© 2024 Keturah Murray. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information.